The postoperative period
Postoperative care begins at the end of the operation and continues in the recovery room or day surgery room, as appropriate, throughout hospitalization and continues during the return home and recovery period.
The main goal of postoperative care is to help the person’s body regain its equilibrium. Postoperative follow-up serves three purposes:
- Ensuring personal safety and comfort upon return from the operating room;
- Permitting optimal recovery and the greatest possible autonomy;
- Preventing possible complications from the operation.
Immediately after the operation, depending on the type of surgery, the medical team checks:
- Respiratory, cardiac and renal functions (by regularly recording vital signs, oxygen saturation, urinary elimination and by observing and monitoring for signs of complications);
- The wound, dressing, drains, intravenous infusions and any urinary catheters that may have been put in place;
- The presence of pain and its intensity in order to relieve it effectively;
- The patient’s mental and emotional state.
Monitoring tests such as an electrocardiogram (ECG) or a blood test may be requested by the surgeon or a consulting physician depending on the individual’s general condition and medical history.
Phlebitis, also known as deep vein thrombosis (DVT) (i.e. the formation of a clot in a vein), is monitored and prevented by administering preventive treatment to patients who are obliged to lie still for long periods of time.
Postoperative pain control
It is normal to experience pain after surgery. This is often worse in the first 24 to 48 hours and gradually diminishes afterwards. The healthcare team is there to help the person get the most effective relief. The nurse will assess the pain throughout the hospital stay. The pain is rated on a scale from 0 to 10, with a value of “0” for no pain and “10” for the worst pain.
Example of a pain scale from 0 to 10:
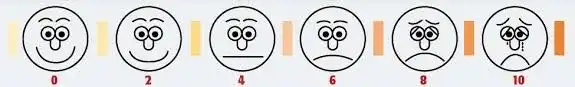
It is important for the pain to be relieved. It helps the patient recover more quickly and prevents complications. Having less pain makes it easier to move, breathe, sleep and eat.
These are the types of medications that may be used for pain relief following surgery:
Patient-Controlled Analgesia (PCA)
Medication administered as needed using a pump connected to the intravenous infusion. When pain occurs, the patient presses a button on the controller connected to the pump. A small amount of medication is then injected. This pump is simple and safe to use. It is programmed not to exceed the dose prescribed by the doctor.
Epidural analgesia
Medication administered continuously through a catheter in the back close to the spine. As described in the previous paragraph, a lever connected to the pump that administers the medication can be used as needed for certain surgeries.
Subcutaneous analgesia
Medication administered by injection under the skin prescribed as needed at intervals determined by the physician. It is recommended that the patient ask the nurse for this medication as soon as the pain starts so that it does not become too severe and thus more difficult to relieve.
Oral analgesic tablets
This type of medicine, taken orally, should be administered as soon as possible. It should also be requested directly upon the onset of pain. This allows the health care team to make sure that the medication relieves the pain well before the patient returns home. When a patient leaves the hospital with medication for at-home pain relief, analgesic tablets are most often prescribed. Analgesic medication that is given postoperatively may cause side effects, including nausea and constipation.
To control nausea, the doctor will prescribe medication that will be administered by the nurse as needed, hence the importance of reporting this adverse reaction to the nurse.
In the event of constipation, here are a few guidelines, if so instructed by the doctor, easily applicable at home, to prevent and better manage it:
- Drink plenty of water (6-8 glasses per day);
- Eat fruits, vegetables and whole grain cereals;
- Consume hot drinks: broth, soup, herbal tea, weak tea to help stimulate the intestines;
- Eat meals and snacks at regular times;
- Perform light exercise (walk after a meal).
The nursing staff will take appropriate steps in order to prevent post-operative complications.
Early mobilization
It is recommended that the patient move every 2 hours when lying down.
The first time the patient gets out of in bed, it should be with the help of the nursing staff, who will use a safe technique to help them get out of bed the first time. It is recommended that patients follow instructions carefully and avoid trying to get out of bed alone.
Breathing exercises
These help eliminate secretions after surgery and thus avoid pulmonary complications such as respiratory infection (pneumonia). It is recommended that these be performed 5 times an hour with or without a spirometer (a device that facilitates deeper breathing), using the following technique:
Without spirometer
In a seated or semi-seated position, place your hands on your stomach.
Breathe in slowly, inflating the belly and hold your breath for 3 seconds.
Exhale slowly through the mouth.
If breathing exercises cause pain due to a stomach wound: use a pillow or folded blanket to put pressure on the wound when exercising or coughing.
With spirometer
In a seated or semi-seated position, exhale to completely empty your lungs.
Place the mouthpiece of the device in your mouth.
Take a slow, deep breath to lift the ball in the device for about 3 seconds.
Circulatory exercises
Circulatory exercises help blood circulation and reduce the risk of blood clots in the veins (thrombophlebitis). It is recommended that they be performed several times an hour using the following technique:
- Lying on your back, take a deep breath;
- Point your toes as far as possible and then pull your feet vigorously towards your chin;
- Breathe out slowly.
Resuming eating
Eating should be resumed as soon as possible yet gradually, depending on the type of surgery, while observing appropriate precautions.
Hygiene
If necessary, assistance will be provided for hygiene care until your gradual return to autonomy.
Urinary and intestinal elimination
For some surgeries, a urinary catheter (a flexible tube in the bladder for emptying urine) will be inserted postoperatively. This may be required from 24 hours to a few days. It allows the bladder to be emptied and kidney function to be monitored.
When eating is resumed gradually, gas may be produced. It is normal to have no bowel movements for the first few days.
WARNING!
It is important to tell the nurse if it is difficult or impossible to urinate and if any discomfort or constipation occurs.
Rehabilitation program
Some operations can cause temporary or permanent sequels or medical complications that require rehabilitation. Rehabilitation should be started as soon as possible after the operation by specialized professionals such as physiotherapists, occupational therapists, nutritionists or others.
Teaching self-care
Self-care is the care the person gives to themselves (for example, do-it-yourself actions to promote wound healing).
When necessary, the nurse will introduce a self-care education program as soon as the person’s condition permits. This often involves learning how to care for wounds or drainage devices (drain, urinary catheter, ostomy care, etc.). The patient will put this knowledge to use upon their return home after hospitalization for a variable length of time, whether on a temporary or permanent basis. Depending on particular needs, some people may be referred to the CLSC in their region for specific care or supervision.
Returning home
Planning the return home
Planning for the return home begins as soon as the dates of the surgery and the expected recovery are known. These are a few recommendations to ensure you are well prepared:
- Arrange things at home so as to make your convalescence as easy as possible. For example, facilitate movement by removing unnecessary furniture or objects. Install larger bedside tables near your bed and chair that can hold everything you need to be comfortable.
- If possible, it is recommended that you prepare meals in advance and freeze them. They will be ready when you return home.
- Make the necessary purchases at the grocery store and drugstore.
- Make sure you have a supply of acetaminophen (Tylenol) for postoperative pain relief.
- Make sure you have a thermometer at home to check your temperature when needed.
- Consider calling on community support services such as: housekeeping, meals-on-wheels, etc. You can get information on these services by calling 211 in certain areas covered by the service or by consulting the “Community and Social Resources” section in the yellow pages of your telephone directory.
- If the home help is insufficient or if the general condition of the patient so requires, you may be able to book a stay in a convalescent home: information is available in the “Retirement Homes for Seniors” section in the yellow pages of the telephone book or on the website of the Ministère de la Santé et des Services sociaux.
Return home and convalescence
In the days or day before release from hospital, the nursing staff or the surgeon will advise you of the possible date of departure. As soon as your planned departure date is known, it is important to notify family and friends in order to plan the return home, accompaniment and transportation. One person will have to stay with you for the first 24 hours. It is the patients’ responsibility to organize their transportation with their loved ones. People who leave the hospital after surgery are generally able to take care of themselves on a daily basis. You may, however, need help with household activities such as cooking, cleaning or shopping.
Ideally, departure should take place early in the day—in the morning, if possible. Here are some important questions to clarify before you leave:
- Previous medication: stop, resume or continue?
- New medication: take for how long?
- When to schedule your follow-up appointment with the surgeon?
- Ask for a summary of the hospitalization to send to the family doctor.
- When should you see your family doctor again?
- Will you need prescriptions for specific medication, wound care or nursing intervention?
- When should you take a shower? A bath?
- When can you resume normal activities and sports?
- When can you start driving again?
- When can you go back to work?
Before leaving the hospital, make sure you have your health insurance and hospital cards to hand, as well as all necessary medical prescriptions and personal medication.
Healthcare personnel will provide clear written or verbal instructions. The information should be tailored to the individual and the clinical situation. Among other things, they will advise the patient or caregiver about the signs and symptoms they should look out for, if relevant, and to notify them accordingly. If there is a request for home care, a liaison nurse will inform the person of the planned follow-up and the date of the first home care visit by the home care nurse.
Pain relief at home
The health care team will provide instructions on the use of analgesics and will issue a prescription if necessary. It is important to relieve pain. The pain will gradually subside, and the analgesic medication will also be reduced until the pain stops. As soon as the pain is less severe, take acetaminophen (Tylenol) rather than another analgesic for as long as it is effective. Follow the prescribed or recommended dosage carefully.
Wound and dressing
For wound and dressing care or postoperative recovery exercises, you should follow the surgical educational guide or the instructions specified by the nursing staff. If more complicated care is required, a request may be made to the CLSC. Nursing staff will travel to the home for people with reduced autonomy, but those who can travel will be attended to by appointment at the CLSC offices.
The surgical wound should be kept out of the sun for a period of 12 months.
Hygiene
Follow the surgeon’s instructions and the educational guide. Avoid getting the wound wet until it is completely closed. Make sure you are familiar with specific instructions for showering or bathing.
Physical activity
Follow the surgeon’s instructions and the educational guide. Avoid strenuous physical effort and activities. Physical activity is essential for recovery and renewal of energy, but must be resumed gradually in order to maintain a balance between activity and the rest required for convalescence. Avoid overexertion by having several short periods of activity rather than one long one. Consult our kinesiologists as needed.
Back to work
The doctor will determine when you can start work again. If you have to stop work during your convalescence, provide the insurance documents required by the employer so that they can be completed by the surgeon. When you are fit to return to work, you are advised to take advantage of gradual return-to-work programs if these are available at your workplace. At the appropriate time, it will be up to the surgeon to specify the terms for a progressive return to work.
Complications to watch out for
Call Info-Santé at 811, the oncology pivot nurse (if applicable), the Info-cancer Hotline at 1 800 363-0063 or go to the emergency room if one or more of the following symptoms occur:
- Pain that increases even with medication;
- Signs of wound infection such as: increasing redness, swelling, pus discharge, pain, heat;
- Fever: Oral temperature for adults under 65 years of age = 38.5°C (101.3°F) and above; for adults 65 years of age and over = 37.8°C (98.6°F) and above;
- A lot of blood on the dressings;
- Inability to eat or drink;
- Vomiting;
- Burning sensation when urinating;
- Difficulty or inability to urinate;
- Constipation unresolved after following instructions issued by personnel upon departure;
- Swelling or pain in a calf that increases with walking;
- Shortness of breath (dyspnea);
- Chest pain;
- Other signs and symptoms listed in the surgery-specific educational guide.
In case of emergency, call 911.
Duration of convalescence
Convalescence is the time after the operation during which recovery is achieved, with a gradual return to health. Its duration varies greatly, from a few weeks to a few months. It varies according to the age and overall health of the person, the type of surgery performed, the rehabilitation required and the type of anesthesia used. However, regardless of the type of surgery performed, it is normal to feel tired. The body mobilizes resources to work on healing and this requires a lot of energy. It is therefore necessary to rest and gradually resume activities in accordance with the energy available. If you are concerned about prolonged fatigue, it is recommended that you inform your health care team or contact the oncology pivot nurse (if necessary) or the nurses at the Info-cancer Hotline at 1 800 363-0063.
Sources (in French only):
Soins post-opératoires
Surveillance post-opératoire
Les exercices respiratoires après une opération
Spirométrie incitative
Sources:
Surgery in cancer treatment
Cancer Surgery
Surgery to Treat Cancer